Low- and middle-income countries have been struggling with the battle against infectious diseases such as HIV/AIDS, tuberculosis and COVID-19. A considerable amount of time, money and effort has been invested into these battles, but these investments did not yet lead to a sustainable and long-term solution. We can take action by using smart innovations, real-time data and improved access to medicines so that we can strengthen the position of low-and middle-income countries in their struggles against infectious diseases.
Introduction
After more than two years of intensive COVID-19 measures, one might forget that there are multiple other infectious diseases still raging through especially low- and middle-income countries (LMIC). Recent publications focus on the cases of HIV/AIDS and Tuberculosis ([WHOE21]), the WHO Regional Office for Europe urges countries to keep investing in battling these diseases after millions of cases are expected to have gone under-diagnosed and under-reported due to the focus on the COVID-19 pandemic ([WHOE22]). Battling these diseases is a challenge. The need for reliable information and access to treatment and medicines is paramount in LMIC.
How does this impact developing countries?
For several decades the international community has invested in LMIC health sectors through multilateral organizations, foundations and governments. This is spread between funds spent on health commodities such as vaccines, medicines and protective equipment and on services to strengthen the health systems by increasing medical capabilities, increasing private sector engagement, building in-country supply chains, etc. ([Bend17]).
Even though much has been achieved, the current global health supply chain is not delivering the desired availability of medicines. Patients are still faced with inadequacy of high-quality medicines, especially in remote health facilities, while at the same time central and regional warehouses are overstocked with sought-after medicines. These congested national supply chains result in unnecessary waste and patients lacking access to required medicines. It has become clear that these issues are not easy to fix and certainly not in a short timeframe.
What are we doing about it?
Over the past years, more technical solutions have been implemented in the global health supply chain. This ongoing digitization allows for the introduction of advanced innovations, especially in the most difficult-to-reach areas of the countries in need. In this article, we will dive into how we solved some of the challenges facing the global health supply chain using digital solutions and what we believe is required from the international community.
The Global Health Supply Chain; Setting the Scene
Before we dive into solutions to improve the healthcare situation in LMICs, we need to set the scene of the Global Health Supply Chain. The Global Health Supply Chain can be split in two distinct parts: the upstream and downstream legs. Upstream medicines are procured from pharmaceutical companies, financed by donors, and transported to a country’s central medical store (CMS). Downstream is where the goods are transported from a country’s CMS to provincial and district warehouses and from there to local healthcare facilities and community health workers.
Especially in the downstream leg, a wide range of challenges can be identified. For different healthcare programs, we encounter parallel streams of funds, aid, and data. Certain medicines, such as the COVID-19 vaccines, require storage at low, sometimes sub-zero, temperatures. Medicines for seasonally occurring infections, such as Malaria, require adequate outbreak response distribution in the wet season. HIV/AIDS treatment requires recurring doses to remain effective, so a constant supply based on the number of patients is essential.
Across the supply chain, numerous stakeholders collaborate to deal with the global, national, and local challenges that supply chains face. While each of these stakeholders have different focus areas, one of the key requirements all of the stakeholders share is reliable data. This data is used to gain insight into funding effectiveness, health status of citizens and to manage the health supply chain effectively. In most countries, supply chain management systems have been implemented on a central and regional level. In countries like Kenya, Tanzania, Ethiopia, Zambia, Zimbabwe, Sudan, Uganda and Nigeria, part of the supply chain is visible. Especially the “Last Mile” (down to the healthcare facility) is still 95 percent paper-based and therefore lacks reliable data that can be used for the above stated purposes. Many countries are struggling to digitize the Last Mile and to increase efficiency in Last Mile distribution ([Spis14]).
In the following sections, we will explain the most striking challenges within the global health supply chain.
Figure 1. A high-level overview of the global supply chain for health commodities to low- and middle-income countries that differ from supply chains in high income countries especially in their reliance on manual labor and the lack of even the most primitive infrastructure such as addresses and roads. [Click on the image for a larger image]
Financial incentives
Typical donor-funded budgets have a limited lifespan. These budget “hand-overs” can often disrupt procurement cycles that should be uninterrupted for effective supply chain management. Ministries of Health of LMICs want to maximize procurement of medicines once funds are available and procedures are met. Therefore, they place typically large and infrequent procurement orders to bridge the medicine supply for future demand. Additionally, warehouse managers are often incentivized to keep warehouses full, which results in overstock and waste due to expiry of old products. Although this is easily turned around by a performance-based incentive ([Spis14]), it is important that the right data is available to make performance-based incentivization possible.
To become eligible to receive funding, LMICs are faced with required reporting templates and information systems that can be different for every donor program. Also, managing multiple supply chains operating in parallel adds additional complexity, whereas multiple donors can sometimes fund similar or even the same commodities ([Pisa19]). Not only is it inefficient to run parallel supply chains; the situation acts as a deterrent to enact real change through digitization. Therefore, donors have started coordinated their funding amongst each other in global donor communities since a few years.
Demand, supply & inventory management
A well-functioning supply chain is important for managing health outbreaks across a country. Unlike in developed countries where the private sector takes care of most of the supply and demand planning for health commodities, in low- and middle-income countries these tasks are performed by a mix of non-governmental, public, and private organizations. This results in a large group of professionals with the best intentions aiming to plan demand and supply separately from each other, with limited collaboration and non-existent real-time information on downstream demand, activities and inventory levels incurring delays, stock-outs and other inefficiencies.
This lack of transparency is largely caused by two factors:
- Parallel operating supply chains with different registration requirements (as mentioned in the paragraph above) and, most importantly
- high prevalence of paper-based registrations.
Paper-based registrations are notoriously less cost-efficient (especially slower) and produce more mistakes than digital (f.e. web-based) data-capture methods ([Webe05]). But, with limited technology penetration in healthcare facilities and district warehouses, paper-based methods are the only methods available. In the current set-up, registration forms are completed by healthcare professionals and submitted once a month to a district facility or larger healthcare facility. These forms – typically in the order of 30 to 50 pages long – are then transcribed and combined with registrations from other facilities in the region into aggregated district registrations. Data is copied, digitized, and aggregated once or twice. The information is 2 to 4 months old at the time it reaches the national level.
The typical Enterprise Resource Planning (ERP) solutions used upstream and by companies in developed countries, are not suitable for healthcare facilities and district warehouses as they are too comprehensive, complex, and expensive. Furthermore, commercial models with recurring license fees often cause a considerable burden on limited financial resource in developing countries. The responsible ministries would rather settle for a system with less functionality that doesn’t require recurring fees, as a one-off fee for implementation is more easily funded by one of the multilateral agreements or international donors. This has resulted in a large amount of open-source implementations of electronic Logistical Management Information System (eLMIS) solutions, which have had mixed results. Most implementations take a lot of time and are very expensive due to the large volume of customization required. Furthermore, since all implementations are very different, there is no easy way to ensure interoperability, for instance with DHIS2.
Logistics management
Managing logistical flows is another component of the global health supply chain that requires some improvements. In the upstream leg, global pharmaceutical companies that currently provide the bulk of medicines had not yet standardized the way data is exchanged with donors, procurement service agents and in-country stakeholders. The typical e-mail with an Excel attachment is error-prone and should be a thing of the past. Only recently, the larger donors have pushed for their suppliers to adhere to the GS1 data standards. We know from markets in developed countries ([Rijs17]) that not all suppliers and vendors that are connected through the GS1 network do deliver high-quality data. Therefore, it remains a topic of interest to ensure that the whole supply chain has reliable and timely end-to-end data.
In-country logistical parties receive shipments on a (bi-)monthly basis, especially those that operate in rural areas in the Last Mile. Incentives are lacking to increase replenishment frequency from once a month to either when stock levels are low or simply to more frequent deliveries. Since the costs for multiple “milk runs” would exceed the fees they receive, this will not change unless something fundamentally alters their business model. Digital innovations will offer a way to enable these organizations to operate more efficiently.
Performance management
Throughout the previous sections, we have explained how the lack of timely and accurate data is a major issue. When reliable data is available, the performance of the supply chain and therefore the health status of the countries can be improved. Typical solutions focus on a large number of logistic hubs to be connected through the same system across a country. This allows the national supply and demand coordinators to easily combine the information in simple dashboards or more elaborate reports.
The downside, however, is that especially the health professionals that are dispensing medicines to patients do not get included in eLMIS implementations and therefore cannot be included in the data-driven supply chain improvement initiatives at all. Training on relatively complex LMIS systems of the large numbers of health professionals that mostly speak local dialects and ensuring hardware availability dispersed over wide rural areas provides major obstacles.
So, how do we ensure that the data that becomes available is accurate, timely and efficiently gathered? How do we prevent one-size-fits-all IT system implementations that lack flexibility and interoperability? And how do we ensure that when users have insights, these insights are interpreted correctly?
We require an integrated approach to tackle all three questions simultaneously ([Okeb20]).
Digitizing the Last Mile in low- and middle-income countries
To improve the global health supply chain, an innovative information system infrastructure is needed. However, there is not a single silver bullet that will solve all issues at hand at once. Organizations across the global health supply chain have attempted to develop technological solutions to solve the challenges mentioned, but most solutions have come up short due to high organizational complexity and low technology penetration in the relevant countries.
We have identified and tested a four-step approach to successfully digitize the Last Mile in low-to middle-income countries:
- Make data available and reliable
- Share data effortlessly
- Interpret data collectively
- Take action
In the following sections, we will elaborate further on our four-step approach.
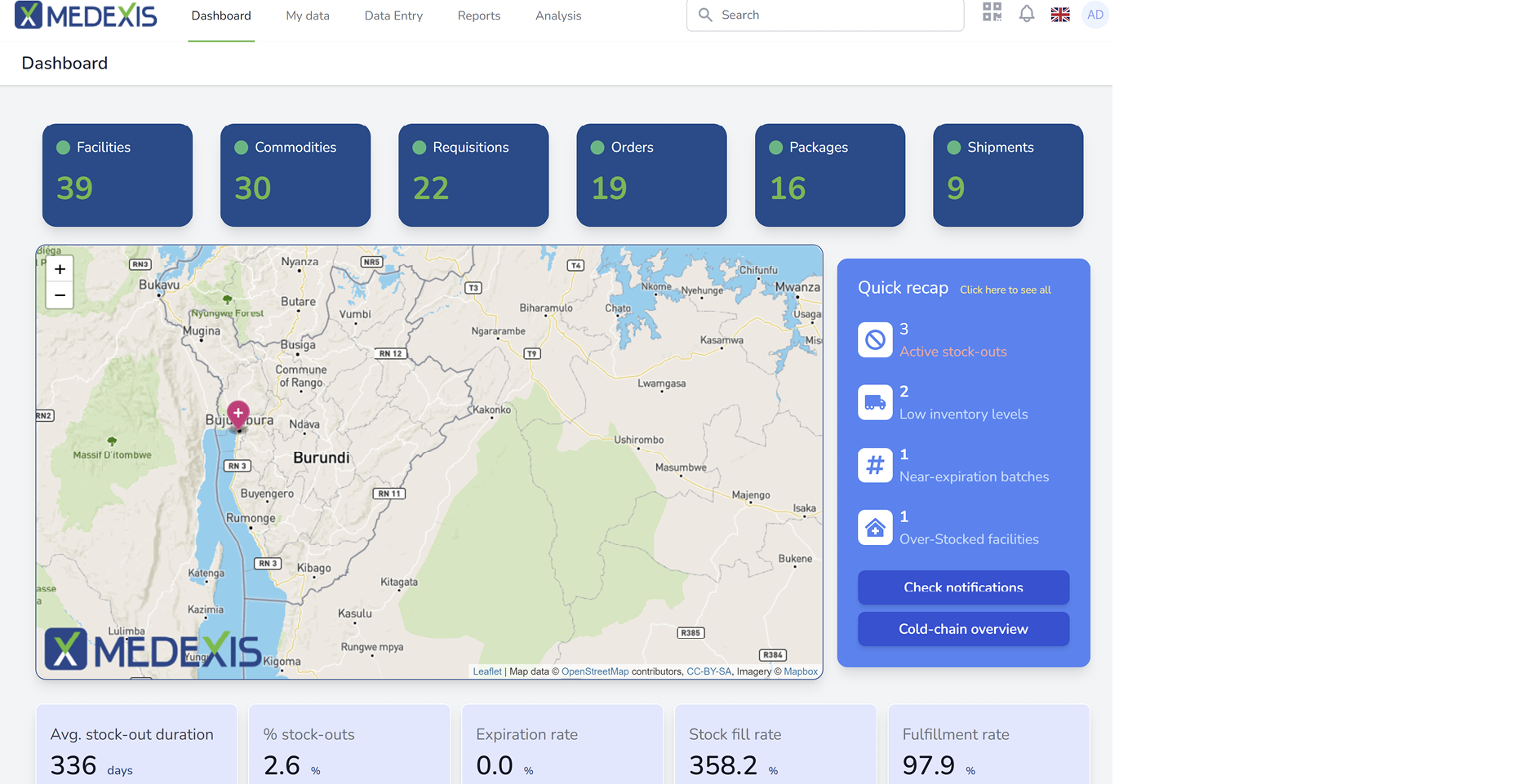
Figure 2. A snapshot of a Medexis LMIS screen that offers easy data entry and viewing of stock levels and outstanding orders. [Click on the image for a larger image]
Make the data available and reliable: low complexity but standardized applications and simple mobile apps
Available and reliable data is the foundation of a digital solution across the global health supply chain. Effort should be put into creating reliable data by digitizing the “paper trail” that is used for medicine orders and deliveries. There are three ways to solve this challenge, which we have outlined on the following pages.
By delegating the registration task to data entry experts.
This will not overload current medical and warehouse staff with extra administrative tasks but keeping the registration and exchange methodology the same. However, this will increase the distance between the source of information (typically the nurse) and the acquisition of that information in for example an ERP system. Delegating registration tasks will only lower the speed at which the data is exchanged at district and national levels, decreasing the timeliness and actionability of the data.
By digitizing the paper forms with intelligent solutions.
By digitizing paper forms with cell phones, a lot of the data will arrive at the national and district level timelier and with less errors. This method also ensures low effort of change for the warehouse operators and nurses, as they fill out the forms as they are used to, but only have to upload this to a central data warehouse. This solution has two downsides, the first downside is the limited internet connectivity in many of the rural areas. With regular uploads of photographs, this limited connection will become a problem. The second downside is that the photographs of the forms need to be transformed from image to text manually or digitally. Both digital and manual methods are not fully waterproof.
Simple and easy-to-use applications can serve as a foundation for reliable data acquisition. As an incremental improvement, current forms can be digitized 1 : 1 to keep the look and feel for the nurses and operators. These solutions can upload structured data in minimal packets to deal with bad internet connectivity or wait with uploading until internet connectivity is established.
Several large donors have pre-selected several solutions in 2019 such as OpenLMIS (https://openlmis.org) and i+solutions’ own solution Medexis (http://www.medexis.org) for the warehouse operations data acquisition and storage requirements. Figure 2 provides a snapshot from a Medixis LMIS screen. These solutions professionalize registration for distribution centers and medical stores, but do not solve the problem for medical health workers. They do not always have sufficient bandwidth to manage even an IT system as simple as the aforementioned solutions.
For small healthcare facilities or individual community health workers, a simpler, a more tailored solution is desired. With the increasing prevalence of mobile technology in developing counties ([GSMA19]), it has become easier to provide mobile health (mHealth) solutions to previously unreachable local health actors such as community health workers and patients themselves.
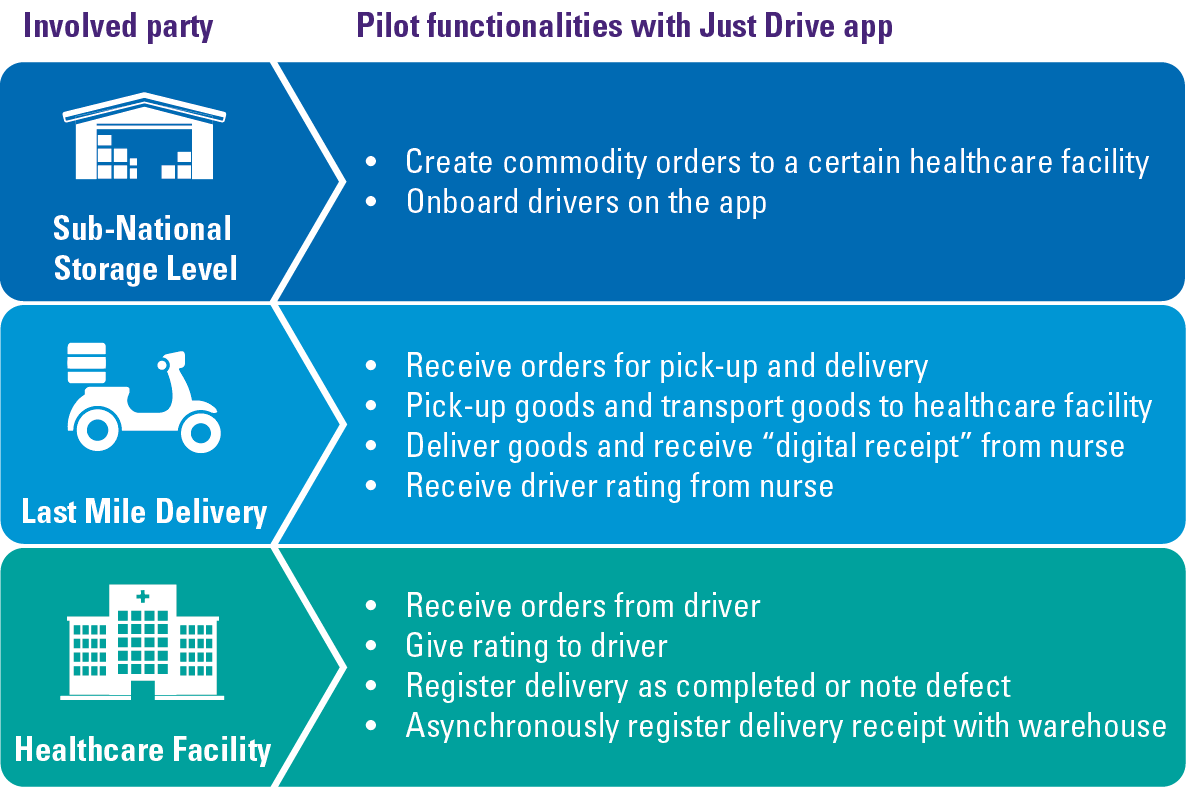
Therefore, in 2021, i+solutions, E-Gateway and KPMG initiated a pilot project to test a mobile “Last Mile” app in Burundi. This app was brought to one district warehouse in Kirundu (Burundi) and eight surrounding healthcare facilities in a 30 km radius. The goal was to prove that simple mHealth applications could improve replenishment and community participation in the last mile supply chain. The application basically covers all the parties in the last mile of health commodity delivery: the district warehouse, the last mile delivery and the health facility. The tasks that the app supports are displayed in Table 1.
The “Just Drive” eHealth solution was piloted with different actors in the supply chain. The district warehouse employee was able to create orders on the app, while certified motorcycle drivers could accept that order and deliver it to the respective healthcare facility. The nurse, in turn, could accept the shipment, note visible defects, and rate the driver’s performance.
Of course, we knew that mobile solutions could be an effective tool in rural areas of developing countries ([Fero20]), so the primary goal of the pilot was to especially learn the effect of these simple mobile apps on the challenges in the Last Mile. How easy could we engage local health professionals and couriers with the application and platform? At the same time, we were also testing the ease of use of the apps and the effectiveness of the low-payload Data Space platform. Finally, we tested the level of digitalization and visualization that we could obtain in the Last Mile and the frequency increase from monthly to weekly for replenishments in rural areas.
After an initial pilot phase of 6 months, the project received very positive feedback and is now being rolled out on a national scale to facilitate all district warehouses and healthcare facilities. The “Just Drive” mHealth solution was piloted with different actors in the supply chain. The district warehouse employee was able to create orders on the app, while certified motorcycle drivers could accept that order and deliver it to the respective healthcare facility. The nurse, in turn, could accept the shipment, note visible defects, and rate the driver’s performance.
Table 1. The functionalities included in the “Just Drive” pilot. [Click on the image for a larger image]
It is, however, essential to not provide mHealth solutions in isolation. Without appropriate solutions for semantic and technical interoperability, none of these solutions can sufficiently scale and make an impact beyond a few local communities ([Berg15]). Interoperability is a huge challenge for the large nation-wide implementations of LMI systems.
LMICs have been struggling with similar data exchange challenges for decades. Typically, these challenges occur in often large, but isolated ecosystems such as the mobility sector (through the Open Mobility Foundation’s Mobility Data Specification (MDS)) or the financial sector in Europe (through PSD2), or the real estate sector in the Netherlands (through the National Association for Realtors and Appraisers (NVM)). However, regardless of their size or complexity, they all have a shared set of agreements and a set of specifications as to how the data is to be structured and shared to which the participating organizations have to adhere to.
Together with the Just Drive mHealth pilot in 2021, as discussed above, our consortium has piloted a data exchange solution to prove data sharing can fulfill the following needs:
- Affordable
- Simple to connect to
- Locally produced, and
- Open to all.
This solution ensures cost-effective universal connectivity to data consumers and data producers and ensures data producers can easily control which parties have access to their data and for which period. After a successful first implementation in rural Burundi, the next step is to scale to the national level, connecting all rural healthcare facilities, warehouses and commit motorcycle drivers to all facilities. We also seek to introduce and connect a patient app that will help patients improve their consumption scheduling and replenishment effort.
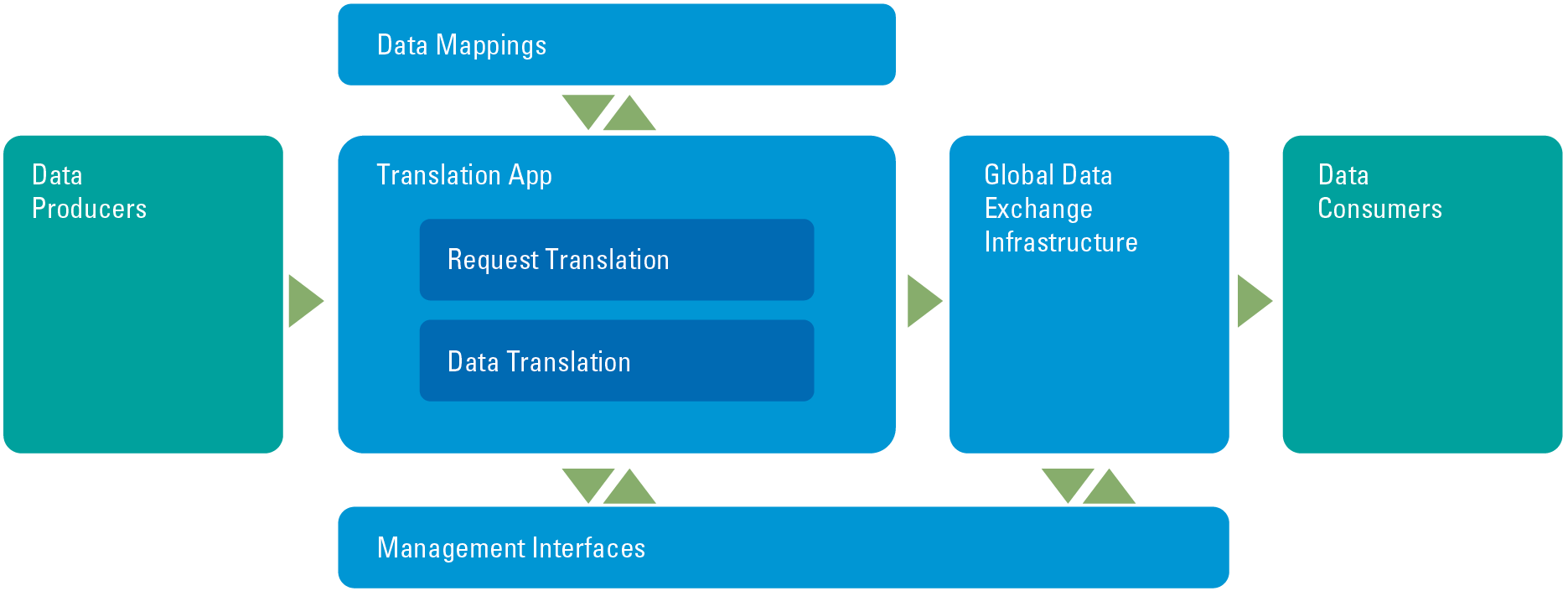
In the future, the data exchange solution, as shown in Figure 3, must contain four basic architectural building blocks; the global data exchange infrastructure that authenticates and routes requests from consumers to the appropriate producer; the management interfaces to set appropriate access rights to datasets or set of records; a translator app that translates requests and data from the available standards, and last the mappings that ensure the translation between standards. These mappings are extensible with “local” variants, ensuring that also different implementations of a system can exchange data.
Figure 3. A conceptual view of the data exchange solution developed to make sharing data easier. [Click on the image for a larger image]
Interpret data collectively: reporting in local and national coordination towers
When high quality data is available and effectively shared throughout the ecosystem, it is not going to provoke action automatically. The next step in the chain is to create appropriate insights. There is not just one stakeholder interested in insights. Depending on the stakeholder, different performance indicators and overviews are relevant. Some examples:
- Donors want to know how much impact is made per USD spent.
- The Ministry of Health wants to know how many patients have been diagnosed and successfully treated with the medicines provided.
- The Central Medical Stores operators want to know which commodities they should order and when to replenish each district warehouse and have operational data to manage the quality of operations.
- District warehouses want to know which commodities should be requested from the Central Medical Stores, to view expected demand from healthcare facilities and to have operational data to manage the quality of deliveries.
Depending on the complexity of the actor and supply chain, different options to visualize the above-mentioned examples are possible. We believe that there are two main categories for visualizing data in the supply chain for such situations:
- Simple visualizations that only deliver actionable insights, and
- More elaborate applications that deliver actionable insights, but also allow a user to run predictive algorithms on the supply chain and other external data to predict the effect on the supply chain.
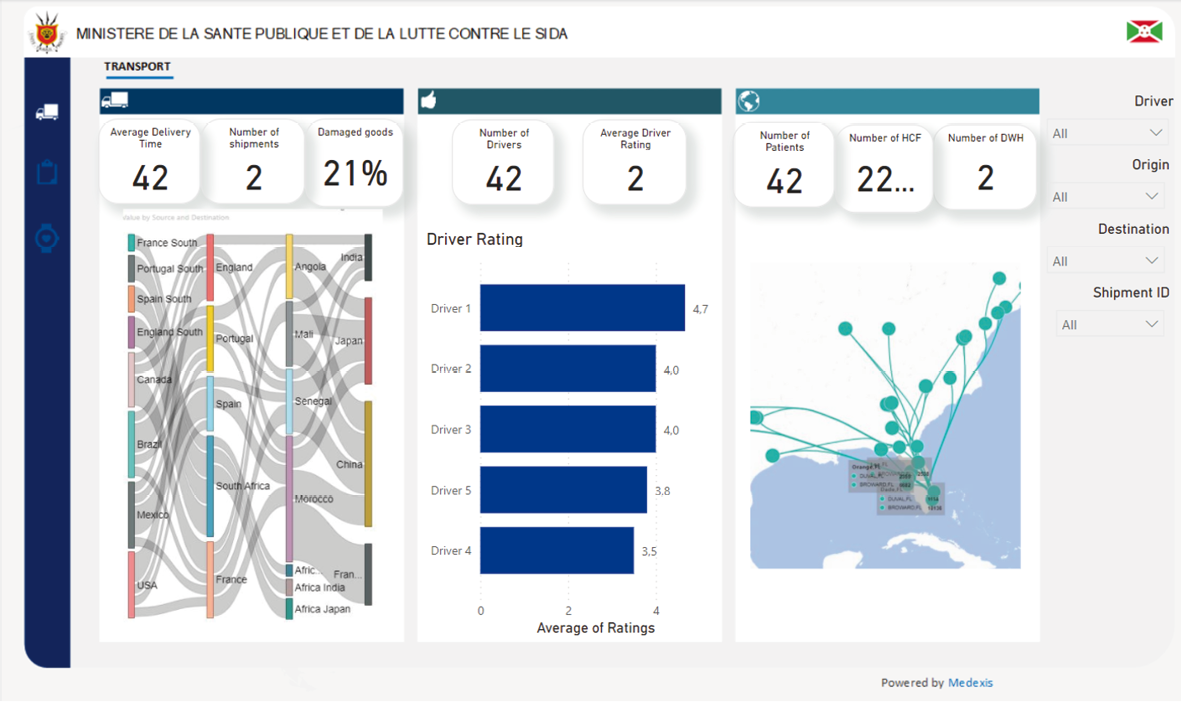
Figure 4. Low complexity data visualization of key performance indicators used to show the flow of physical goods. [Click on the image for a larger image]
The PowerBI dashboard (see Figure 5) that is used for the Burundi Just Drive pilot is very simple in that it displays supply paths, anonymized driver ratings and several key performance indicators relevant for the district warehouse employee to manage the drivers and warehouse operators.
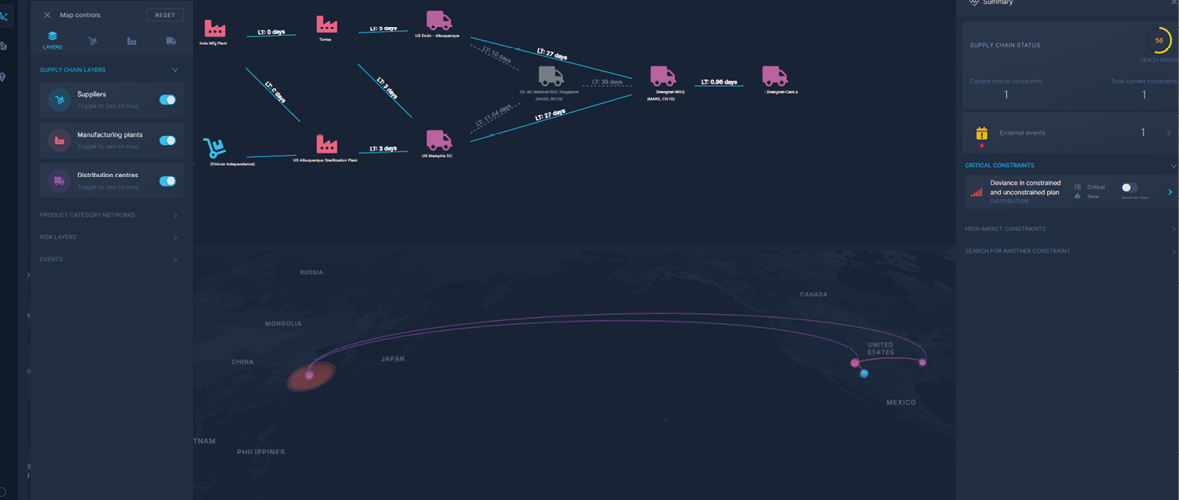
Figure 5. A more elaborate coordination tower solution: KPMG’s Supply Chain predictor. [Click on the image for a larger image]
Conclusion: take action
With smart innovations, real time data and improved access to medicines, LMIC’s health supply chains can be strengthened. Action must be taken based on the insights to improve operations across global health supply chains. Therefore, it is essential to provide easy tooling for local stakeholders through programs tailored for supply chain operations in these rural areas.
As an NGO that is active in the field of supply chain innovation for global health for low- and middle-income countries, i+solutions is committed to improving access to medicines for all patients. In the past years, i+solutions has concluded a wide range of interviews and analyses, pinpointing the major obstacles that prevent the global health supply chain from providing full access to medicines for patients in LMICs. Based on this analysis, i+solutions has been cherry picking and testing recent technologies that can break these obstacles through smart implementations that address the limitations that are so specific for these countries. KPMG is invested in creating a more equitable world. Especially with the COVID-19 outbreak still on top of mind, the lessons learned from dealing with this disease should be applied to the challenges in developing countries. Through KPMG’s long-term commitment to the KPMG Impact program, we are committed to investing in enabling sustainable change across the environmental, social and governance topics. With our work in the global health supply chain, we aim to make impact to the health of billions and solve some of the largest challenges of our time.
References
[Bend17] Bendavid, E., Ottersen, T., Peilong, L., et al. (2017, November 27). Development Assistance for Health. In: D.T. Jamison, H. Gelband, S. Horton et al. (Eds). Disease Control Priorities: Improving Health and Reducing Poverty, 3rd edition (Chapter 16). Washington (DC): The International Bank for Reconstruction and Development / The World Bank. Retrieved from: https://www.ncbi.nlm.nih.gov/books/NBK525305/
[Berg15] Bergstrom, A., Fottrell, E., Hopkins, H., Lloyd, D., Stevenson, O., & Willats, P. (2015). mHealth: can mobile technology improve health in low-and middle-income countries. UCL public policy briefing. Retrieved from: https://www.ucl.ac.uk/public-policy/sites/public-policy/files/migrated-files/mhealth_briefing.pdf
[Fero20] Feroz, A., Jabeen, R. & Saleem, S. (2020). Using mobile phones to improve community health workers performance in low-and-middle-income countries. BMC Public Health, 20(49). Retrieved from: https://doi.org/10.1186/s12889-020-8173-3
[GSMA19] GSMA (2019). Mobile for Development. The State of Mobile Internet Connectivity Report 2019. Retrieved from: https://www.gsma.com/mobilefordevelopment/resources/the-state-of-mobile-internet-connectivity-report-2019/#targetText=The%20State%20of%20Mobile%20Internet%20Connectivity%20Report%202019&targetText=For%20many%20of%20these%20individuals,%2Dincome%20countries%20(LMICs)
[McDa21] McDade, K.K., Munge, K., Kokwaro, G., & Ogbuoji, O. (2021). Reducing Kenya’s health system dependence on donors, in the Brookings Institution’s Future Development blog. Retrieved from: https://www.brookings.edu/blog/future-development/2021/03/02/reducing-kenyas-health-system-dependence-on-donors/
[Okeb20] Okebukola, P. & Fleming, M. (2020). Transforming global health supply chains through data visibility. McKinsey & Company Article. Retrieved from: https://www.mckinsey.com/industries/public-and-social-sector/our-insights/transforming-global-health-supply-chains-through-data-visibility
[Pisa19] Pisa, M. & McCurdy, D. (2019). “Improving Global Health Supply Chains through Traceability” CGD Policy Paper. Washington, DC: Center for Global Development. Retrieved from: https://www.cgdev.org/publication/improving-global-health-supply-chains-through-traceability
[Rijs17] van Rijswijk, A., van der Ham, R.F., & Swartjes, S. (2017). Data Quality GS1: The importance of data quality in the food industry. Compact, 2017(1). Retrieved from: https://www.compact.nl/articles/data-quality-gs1/
[Spis14] Spisak, C., & Lindsay, M. (2014). Use of Incentives in Health Supply Chains—A Review of Results-Based Financing in Mozambique’s Central Medical Store. Arlington, Va.: USAID | DELIVER PROJECT, Task Order 4, and Bethesda, Md: Health Finance & Governance Project. Retrieved from: https://www.rbfhealth.org/sites/rbf/files/Use%20of%20Incentives%20in%20Health%20Supply.pdf
[TGF19] The Global Fund (2019). Value for Money Technical Brief. Retrieved from: https://www.theglobalfund.org/media/8596/core_valueformoney_technicalbrief_en.pdf
[Webe05] Weber, B.A., Hossein, Y., Rowe, M.A., Weber, J.P. (2005). A comparison study: paper-based versus web-based data collection and management. Applied Nursing Research, 18(3), 182-185 . Retrieved from: http://dx.doi.org/10.1016/j.apnr.2004.11.003
[WHOC21] World Health Organization (2021). Critical preparedness, readiness and response actions for COVID-19. Retrieved from: https://www.who.int/publications/i/item/critical-preparedness-readiness-and-response-actions-for-covid-19
[WHOE21] European Center for Disease Prevention and Control and WHO Regional Office for Europe (2021). World AIDS Day: Concerning number of HIV infections going undiagnosed, new data shows. Retrieved from: https://www.euro.who.int/en/media-centre/sections/press-releases/2021/whoeurope-and-ecdc-joint-press-release-world-aids-day-concerning-number-of-hiv-infections-going-undiagnosed,-new-data-shows
[WHOE22] European Center for Disease Prevention and Control and WHO Regional Office for Europe (2022). Tuberculosis remains one of the deadliest infectious diseases worldwide, warns new report. Retrieved from: https://www.euro.who.int/en/media-centre/sections/press-releases/2022/whoeurope-and-ecdc-joint-press-release-tuberculosis-remains-one-of-the-deadliest-infectious-diseases-worldwide,-warns-new-report